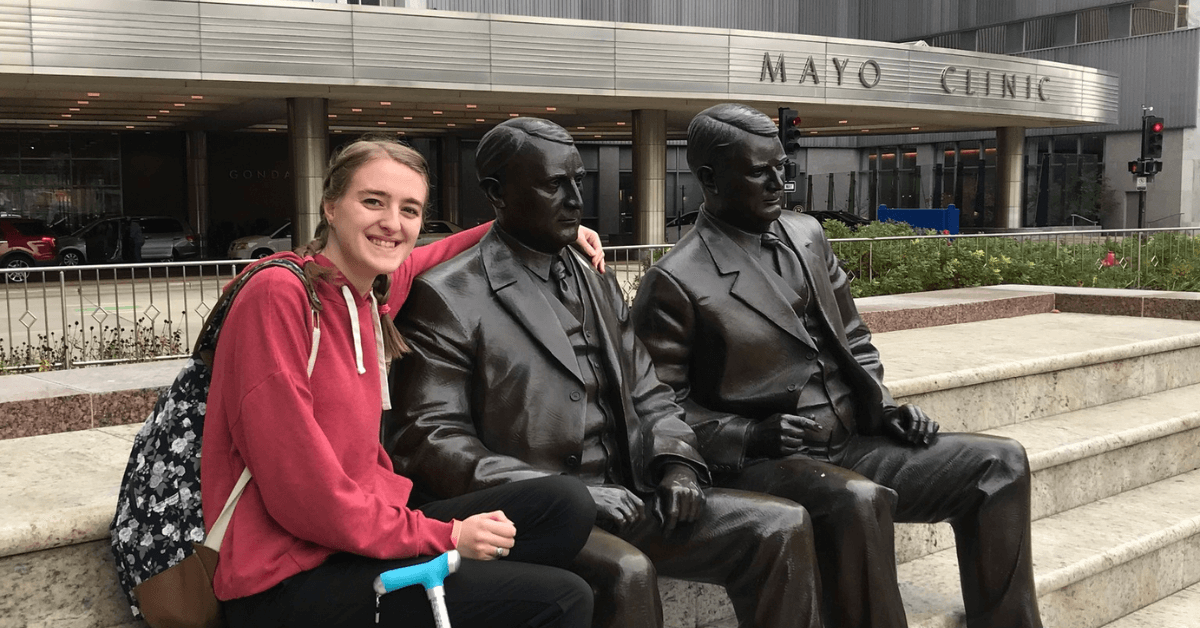
02 Nov Mayo Clinic for POTS – An Overview of My Experience
It finally happened! I have officially received a comprehensive evaluation on my symptoms of autonomic dysfunction and the miscellaneous health issues that have been so debilitating.
I was especially jazzed about this opportunity, because Mayo Clinic is known for their work with people who have postural orthostatic tachycardia syndrome (POTS). In fact, they are the ones who coined the term “POTS”, who set the diagnostic criteria, and who continue to study treatments and long-term outcomes of those with the illness. One of their doctors, Dr. Philip Fischer, has even written a book outlining POTS and how Mayo Clinic typically approaches things like lifestyle recommendations and medications (read my article on his book here). But after following the recommendations and still finding that my symptoms were limiting my daily functionality, I knew I needed help.
How I scheduled my appointment to be seen
Once my symptoms became debilitating in the fall of 2022, I sought help from a local cardiologist, who ordered autonomic testing and discovered I had POTS. He then referred me to a POTS specialist through Froedtert Hospital here in Wisconsin, but the soonest they could see me was in 10 months. I was grateful for the appointment, but genuinely didn’t feel I could wait that long. In the weeks prior, I had requested an appointment to be seen for POTS at Mayo Clinic over the phone (via a number I found on their website), but was told they were not currently taking external referrals, and so I assumed that was a closed door. But when we learned Froedtert would be so far out, we decided to go to a local Mayo systems Clinic, and see if we could get an internal referral. It was a success! She not only succeeded in referring me to the Rochester campus for POTS, but she also helped me try a few different medications in the meantime after consulting with her colleagues. Perfect!
They let me know there was about a 6-month waitlist, and soon enough, I had an appointment scheduled in Rochester for October 2023.
Itinerary details

Two and a half months before my trip, I received an itinerary through the patient portal that outlined my scheduled appointments and tests. First on the docket was a POTS consultation with an RN, followed by a consult with my main coordinating doctor from Internal Medicine. There were many tests throughout the week, and then ended with another appointment with the doctor. About 2 weeks before my trip they were still adding and shifting things, which is important to keep an eye on. If you are planning your trip to Mayo, I would suggest seeing if you can pad your lodging by a day or two on either end, just in case. For us, it was helpful to go a day in advance to check out the buildings, see the parking situation, and get settled into our Air BnB. But we should have allowed extra time at the end of our trip, because when our stay was extended, we had to pack up and stay at a hotel because someone had already booked the next day at our bnb.
As another quick side note, if stairs bother you, be sure to find lodging without them. Even just a few steps can seem insurmountable after a long day of testing. We weren’t able to find an Airbnb without them, but it was definitely a challenge throughout the week.
Initial POTS consult
Here’s a picture of me at my first appointment. I’m holding the LAST loop to my paper chain, signifying that the day has FINALLY come! It was a very exciting moment – one I had been anxiously awaiting for a long and hard season.

My first appointment was with a nurse who did a comprehensive history and symptom evaluation. We discussed my timeline of events and issues over the last few years, and I told her about my symptoms, daily functionality, and hopes for my time at Mayo. She also took me through an extensive list of symptoms to confirm or deny, and then did a tender point test (pressing on 18 places on my body to see if my body interprets pressure as pain, like the sides of my knees, arms, shoulders, neck, and all over) which was very interesting. I was totally surprised to find that every single spot was painful, and when she told me my score was 18/18, I looked at her in confusion and asked “But what does that MEAN?!” She just smiled, and said, “The doctor will discuss more with you later.”
That was definitely the moment I took a deep breath and realized that I was in good hands. These medical professionals are not only aware of POTS, but also the nuances of how it affects all the systems of the body and/or exists alongside other conditions.
Throughout our appointment, she took copious notes, offered compassion, and made me feel right at home.
Next I visited with the doctor. He asked questions about my symptoms and confirmed the game plan. When asked if there was anything else I’d like to discuss, I whipped out my document noting all my concerns. As we went through the list, he quickly added tests to my itinerary. He referred me to neurology for the migraines I had been experiencing, and after hearing more about my miscellaneous symptoms he added lots of blood work for a total of about 14 different panels. Being prepared to discuss ALL my concerns was key, and had I not brought up things that have felt “off”, those things would not have been evaluated. But once we had a plan, I was excited for the week, and ready to find out what exactly was happening, and what we were going to do about it.
The week of testing
During our 8 days in Rochester, these were the tests that I had:
- Autonomic reflex screen
- Catecholamine test
- InBody scan
- Cardiopulmonary exercise test spirometry
- Exercise test
- Echocardiogram
- Brain MRI
- Holter Monitor
- Sleep oximetry
- 24-hour urine test
- Blood tests
In addition to:
- Physical therapy
- Occupational therapy (biofeedback)
- Autonomic dysfunction educational visit
- Neurology consultation
- Evaluation for the 3-week rehabilitation program
Plus additional testing and a referral to another specialist that is still in the works.
As someone who frequently wondered if there was more than “just” POTS going on, I was genuinely excited that I had the opportunity to do all these tests and get to the bottom of what was happening. And yet, as someone who has had a rather severe aversion to doctors and needles for the entirety of my childhood, that excitement was soaked in anxiety.
The most important thing for me, was to stay curious. It crossed my mind MANY times to politely decline certain tests that scared me (like the QSART or the catecholamine test), but I always came back to curiosity. I couldn’t bear the thought of leaving Mayo Clinic, KNOWING there was more to be discovered that I had chosen to skip. I learned everything I could about the tests beforehand, asked lots of questions during the testing, and postured myself as a collaborator in finding answers more than an unwilling participant. Curiosity may have killed the cat, but it saved my trip to Mayo.
If you’re a potsy looking for reassurance as you face certain testing, I want you to know that anything in the above list is totally DOABLE. You can 100% do it. I will be writing articles for each of the tests to offer my tips and thoughts to help you to know what to expect for your own medical adventures, and as I do that I will update the list to link to those articles. So stay tuned, or if you have any questions or concerns in the meantime, reach out through the comments or my “contact me” page and I’d be more than happy to chat.
Using a wheelchair to get around the Mayo buildings

In my day-to-day life I use a cane to help stabilize and support me while standing and walking (read more about that here), but at Mayo Clinic we quickly realized that I needed to be pushed in a wheelchair. The buildings are large, the hallways are long, and the tests can be scheduled one after the other for hours at a time. The fabulous thing, is that Mayo has wheelchairs EVERYWHERE, and EVERYONE is using them. It was quite overwhelming at first, actually. I would say that *most* people had some kind of mobility aid, medical equipment, or other external indicator of serious health issues, regardless of age. It was a lot to take in, but we quickly fit right in, and people didn’t give us a second look.
To the right is a picture of me in a Mayo wheelchair in front of one of the many gorgeous pieces of artwork that line the walls.
Having family along
It was crucial for me to have my mom and grandma along with me. They not only pushed me in the wheelchair, but they kept track of the schedule and timing, got me where I needed to go, acquired food, water, and snacks, dropped me off to park the car, took notes during appointments, and a bazillion other things. It would not have been possible without them.
Also, one of the hardest parts about the testing was keeping track of when I could eat and drink. There were several days that I had to fast, and overlapping testing meant I sometimes wasn’t able to eat for several mealtimes in a row. I felt pretty nauseous and weak for most of the trip, and ended up losing a bit of weight (which was not good, given the fact that I am already underweight and that contributes to worse POTS symptoms). But having a mom or grandma to make, order, or open food was important to consuming calories even when I didn’t feel like it.
Final appointment
I’ll be straight-up honest, and say that my time at Mayo clinic was awesome, but it wasn’t perfect. I made fast friends with staff, LOVED the enormous quantities of information, and genuinely feel like I have a clear path forward in recovering from POTS with central sensitization, migraine, chronic fatigue, and other things we discovered. But at the same time, my main coordinating doctor didn’t necessarily meet expectations. While he gave me great in-person education, prescribed an appropriate medication, and verbalized solid next steps, he neglected to include several important elements in my medical records (like a full list of diagnoses, or the needed accommodations he promised to mention along with instructions for my primary care doctor), and had a pretty strong language barrier that resulted in miscommunication both ways (and a general sense that he was missing details). Overall, I am still needing to be an active advocate for myself, which as you can understand, is very wearying. To ignore the disappointing aspects would be to give an incomplete picture, but while there are parts that I wish had gone better, I am still overwhelmingly encouraged by everything that I experienced and the clear path forward I feel that I have been given.
And the adventure is not over yet. Certain blood and imaging findings are requiring more investigation {Read about the tumor we found and how surgery went here}, and I have another appointment with my main doctor to follow-up on the new medication and to check in and see how things are going {Update: new med is working! Read more here}. I will also be pursuing insurance approval for the 3-week rehabilitation program that I was invited to participate in, which would give me a substantial advantage as I look to reconcile my medically necessary limitations with living an abundant life.
In the meantime, I hope to sort out what I need from my doctor, put into practice the things that I have learned so far, and continue to process what it all means for my life – past, present, and future.
-
Recovery with POTS and CFS
It has been 8 months since graduating from the Mayo Clinic Pain Rehab Program, and I continue to be 85% recovered (depending on the day) from postural orthostatic tachycardia syndrome (POTS) and chronic fatigue syndrome (CFS). I never would have imagined that my health could make such......
28 October, 2024 No comment -
Making a Full Physical Recovery – A Day-by-Day Miracle
“You should exercise more.” A brutal statement. One I had tried to fulfill on my own, and time and time again, had failed. It was a frustrating piece of advice from my doctor, and felt so out of reach as I navigated my bouquet of chronic illnesses....
27 June, 2024 3 Comments -
Awesome Recovery News!!
I am so excited to report that after graduating from the 3-week Pain/Symptom Rehabilitation Center at Mayo Clinic in Rochester and continuing the program at home, I am nearly 100% recovered!...
05 March, 2024 3 Comments





Pingback:The QSART For POTS - My Experience - Kaley Faith
Posted at 14:32h, 22 November[…] went to Mayo Clinic in Rochester, MN to be evaluated for POTS that was not responding to lifestyle changes and was […]
Pingback:What is the Valsalva Maneuver like? - Kaley Faith
Posted at 12:51h, 17 January[…] part of Mayo Clinic’s autonomic evaluation (read more about my experience at Mayo with POTS here), but underneath, it’s one of the coolest and most complicated mechanisms of the human body that […]